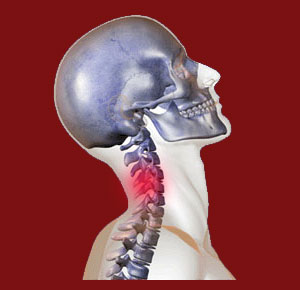
Neck extension facet joint pain ensues when the patient extends their cervical spine, looking upward and moving their occiput towards the upper back. Neck extension is a common movement that is well accommodated by a typical cervical spinal region, but can become problematic in the face of significant facet joint pathology.
We tend to extend our necks when exercising, as well as during many recreational and vocational pastimes. Neck extension might be part of work responsibilities for some types of occupations, such as technicians and manual laborers, and is usually part of domestic cleaning chores, as well.
Why does extending the cervical spine create worsen pain in the facet joints in many affected patients? What types of symptoms are actually generated by this motion? Most importantly, how can patients who experience neck extension facet joint pain find relief without continually aggravating their condition? We will explore of all these important questions during the course of this focused essay.
Symptoms of Neck Extension Facet Joint Pain
Pain associated with neck extension will occur or worsen when the patient looks upwards, bringing the rear of the head closer towards the upper back region. Pain is most often located directly on the center of the vertebral column, although in some cases, the expression of symptoms might be slightly off to one side or both.
Pain might be present upon any extension movement, but this is rare. Far more commonly, patients report being capable of extending the neck to some degree and then suffering pain if they continue past a comfortable range of motion. Usually this occurs between 40% to 65% of total ROM for neck extension.
Pain is likely to be sharp and sudden upon movement, then tapering off quickly to a dull soreness before dissipating completely or nearly completely in most typical patient profiles.
Sources of Neck Extension Pain
Neck extension facet joint pain can occur for identical reasons as neck flexion facet joint pain, which also accompanies extension-related symptoms in many patients. The usual origins of these types of mechanical facet joint pain include the following scenarios:
Osteophytes can form in and around the facet joints, making smooth and pain-free movement a thing of the past. Joint degeneration is a normal part of getting older and usually does not become a pathological concern. However in some cases, spurring can prevent normal range of movement and might cause painful interactions between affected neighboring vertebral bones.
Joint dislocation or fracture can cause pain upon mobilization, typically in a specific range of motion. These injuries might be very subtle and difficult to image, but might be diagnosed through physical exam and range of motion observation in the absence of other more obvious causes of symptomology.
Help for Neck Extension Facet Joint Pain
We suggest that all cases of confirmed or suspected facet joint pathology should receive care from a qualified spinal orthopedist, physical therapist or sports medicine physician. These medical professionals are best suited to manage these conditions successfully, using a combination of conservative, moderate and possibly, surgical interventions. However, for patients who need help right now, we advise the following coping strategies can be both effective and safe:
Try to ascertain the range of motion that is allowable and begin to limit motion outside of this comfortable range. If pain is not too severe, patients might want to slowly try to push past this range, as continued efforts can actually break down some forms of spurring, basically curing the mechanical pain syndrome as is demonstrated in physical therapy evidence. However, movement might result in acutely severe pain and may actually exacerbate arthritis, as well, so patients should always seek out the opinion of their physical therapist before pushing the limits of their pain too far.
Some patients will simply stop moving their neck as much as humanly possible. While this can be highly effective for motion-related pain conditions, the ramifications of such strategies can be terrible. A lack of movement can be detrimental to the soft tissues and joints in the region, causing atrophy, capsule shrinkage and even frozen joints in select case profiles. It is better to try to move as normally as possible, simply avoiding the most severe manifestations of pain by restricting severely symptomatic movement until advised by a doctor.
Note: Do not attempt to “reverse” pain by performing large amounts of neck flexion. This can lead to similar pain upon looking downward, if it does not already exist, and will also contribute to problematic forward head posture conditions.
Facet Joint Pain > Facet Joint Facts > Neck Extension Facet Joint Pain





